Achilles Tendonitis | An Ultimate Guide for Runners
Achilles Tendonitis (or Tendinopathy) is a very common source of agony for runners. Achilles tendon pain when running can be debilitating and here Helen covers the basics of what it is, why it happens and how to treat it.
What is Achilles Tendonitis (Tendinopathy)?
Achilles tendonitis is a common problem, particularly among running and jumping athletes, and if not diagnosed and managed correctly it can become chronic and make even the simplest of daily tasks difficult. Tendonitis is generally an overuse running injury, although it can also occur as a result of a specific injury.
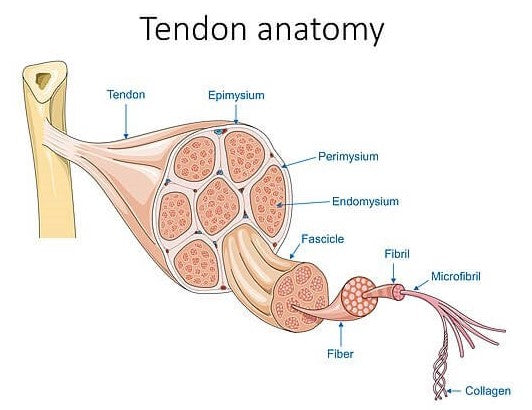
Basic Tendon Structure
Healthy tendons have relatively few blood vessels, but the blood supply can vary between the sites and depending on age. The area with the best blood supply is where the tendon inserts into the heel bone, whereas the area with the least blood supply lies approximately 2-6cm above the insertion, making this area much harder to heal.
In Achilles tendinopathy patients, the tendon appears thickened, uneven and brownish.

Common Causes of Achilles Tendonitis in Runners
There are also several factors that may play a role in the onset of Achilles tendonitis, both hard-wired in the runner (intrinsic) and external factors (extrinsic).
What causes Achilles problems (intrinsic):
- Biomechanical abnormalities – e.g. leg length discrepancy, varus deformity of the foot, restricted subtalar joint, overpronation.
- Systemic conditions – e.g. increasing age, inflammatory arthropathies, corticosteroid use, diabetes, hypertension, obesity, gout.
Causes of Achilles problems (extrinsic factors):
- Mechanical overload and training errors – for example, increased run interval training, excessive hill running training, run training on hard or sloped surfaces, increased mileage and repetitive loading, poor shock absorption.
- Footwear – too old/worn or new shoes not suited to your feet.
Different Types of Achilles Tendonitis
There are two main types of Achilles Tendonitis:
-
Insertional Achilles tendonitis (IAT)
- Occurs at the lower end of the tendon where it inserts into the calcaneus (heel bone)
- Similar to what is known as Severs disease in children.
- Usually occurs gradually although it can be an acute or sudden onset.
- More common in highly active individuals and runners
-
Non-insertional Achilles tendonitis (NIAT).
- Occurs in the middle portion of the tendon, approximately between 2-6cm above the insertion into the calcaneus
- Tends to occur in older, less active or overweight individuals.
What are the Symptoms of Achilles Tendonitis in Runners?
The common symptoms of Achilles Tendonitis that runners usually face include:
- Pain (can be sharp or more of a dull ache)
- Swelling
- Stiffness (particularly first thing in the morning or after a period of rest)
- Visible lump (particularly if it has become chronic)
- Impaired physical function
Many terms have been used to describe the disorder but studies suggest that it is caused by a failed healing response where the tendon has been unable to adapt to the strain being put through it. This failed healing response includes 3 different continuous stages (reactive tendinopathy, tendon disrepair, degenerative tendinopathy). Because there is not an inflammatory response in all stages, the term 'tendinopathy' is more appropriate, but 'tendinitis' is perhaps the more commonly used term among athletes and runners. From a reader’s perspective, we are therefore using the terms interchangeably in this article.
If the source of the tendon injury persists, the area of degeneration or tear may continue or worsen over time. There may also be associated with inflammation of a bursa or other tendon sheaths in the area. It really is important, therefore, for runners and athletes to treat the problem seriously and fix it before it worsens.
How Long does Achilles Tendinopathy Take to Heal Naturally?
There are three phases of repair for an Achilles tendonitis injury.
- The initial Inflammatory phase
- Lasts a few days
- Erythrocytes and inflammatory cells migrate to the injury site within the first 24 hours
- There is also initiation of proliferation of tenocytes and production of collagen fibre
- The proliferative phase
- Begins after a few days
- Synthesis of type III collagen reaches a peak and continues for a few weeks
- The modelling phase:
- Begins after approximately 6 weeks
- Healing tissue is resized and re-shaped.
- This re-modelling phase starts with a fibrous consolidation process where the repair tissue changes from cellular to fibrous, and the collagen fibres align along the direction of loads applied to the tendon.
In the tenth week the injury is considered ‘mature’, and the fibrous tissue gradually changes to scar-like tendon tissue over the course of a year. The quality of the tissue can be weakened if there has been an abnormal healing process.
How to Treat Achilles Tendonitis?
There is no gold standard for treating the Achilles because different clinical studies have shown different results. However, here are some options for improving and managing the pain and difficulties you may be experiencing when running and in daily life:
-
Relative Rest and Moderating Exercise
Initially try to avoid hill walking/running and things that aggravate the Achilles. It is important to modify your training programme and specific exercises.
Pain relief – paracetamol and ibuprofen or gels may allow you to manage the pain so you can keep running and training and some people find ice effective in reducing their pain. Apply the ice for 10-15 minutes at a time, every few hours if required. Please check with your doctor before taking medications.
-
Footwear
Make sure you have supportive footwear with good shock absorbency. You can also try a heel lift in the back of your shoe which will plantarflex the ankle more and in turn offload the Achilles tendon.
-
Massage or Foam Rolling
Work through the calf to relax the muscle and take tension off the Achilles tendon. Deep friction massage and tendon mobilisation can also help to improve tissue elasticity.
-
Kinesiology tape
Apply kinesiology tape to take the tension out of the calf and off the Achilles tendon.
-
Eccentric exercises
Eccentric exercises can help in the early treatment of NIAT in particular. Eccentric strengthening exercises of the calf stiffen and lengthen the myotendinous unit, which decreases the neovascularisation in the tendon.
- Straight leg and bent knee heel drops - 3x15 reps on each exercise twice a day for 12 weeks. Once you can get through these exercises with no pain or aggravation afterwards you can add load.
If you have access to sports massage therapists and medical professionals, you can also try the following:
-
Therapeutic Ultrasound
Therapeutic ultrasound has been shown to reduce swelling in acute inflammatory stages of soft tissue disorders, relieve pain, and increase function in patients with chronic tendon pathologies. Animal studies also show it can stimulate collagen synthesis.
-
Extracorporeal Shockwave Therapy (ESWT)
Studies found EWST might aid in the initiation of tendon regeneration in tendinopathy. There is good evidence that EWST is effective in treating chronic Achilles tendinopathy. However, the most effective doses and duration are still unknown.
-
Corticosteroid Injections
Corticosteroid injections can reduce pain and swelling but may have adverse effects and decrease tendon strength.
-
Platelet Rich Plasma (PRP)
Platelet Rich Plasma inserted at the site of injury can facilitate healing, and it seems that it could also increase collagen types I and III.
Make sure you discuss any medical treatments with your doctor and never attempt to self-administer these home-versions of these treatments.
__________________________________________
Physio Helen Jewell is an experienced sports physio running Ivybridge Physio Fix close to our offices in Devon. She has written a number of articles for us on common injuries and how to prevent and treat them.
Other articles in our physio series by Helen Jewell include:
Calf Heart Attack: https://neuff-red.co.uk/blogs/news/calf-heart-attack-physio-series-by-helen-jewell


Leave a comment